As pandemic restrictions have eased, many Canadians have begun enjoying gathering again with family, friends, and colleagues in a more carefree manner. While smoother waters abound, the reality is that there are many moving parts working hard beneath the surface to keep us safe. Public health is carefully monitoring the Coronavirus disease of 2019 (COVID-19), an infectious disease caused by the SARS-Coronavirus, and its variants.
With limited polymerase chain reaction (PCR) testing available and recognized limitations of rapid antigen tests (RATs), wastewater surveillance has become Canada’s best tool to track emerging cases.
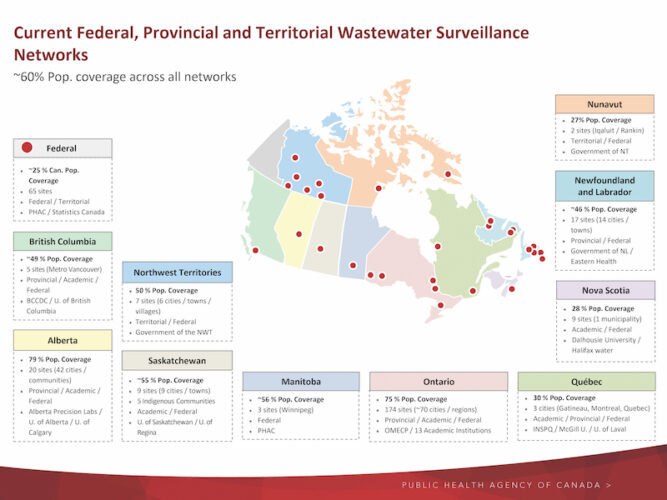
Currently, wastewater testing for SARS-Coronavirus is performed at over 200 sites in Canada, including all provinces and two territories. Internationally, wastewater testing for this virus has rapidly expanded with over 2,200 testing sites in 55 countries.
However, experts warn there are limitations and challenges involved in attaining accurate results.
Wastewater soup
On March 11, 2020, the World Health Organization (WHO) declared the COVID pandemic. While much has been learned about this powerful and contagious coronavirus, it continues to evolve and elude scientists and public health officials. Neary 500 million people have been infected in approximately 200 countries. More than six million people around the globe have perished. In Canada, as of March 25, 2022, there have been almost 3.5 million cases and more than 37,000 deaths related to COVID.
The original virus has rapidly evolved into a string of variants. Fortunately, these can be detected in the stool of infected people over a significant portion of their illness, providing an opportunity to test and monitor wastewater for the presence of COVID in communities and institutional settings without the need for individual testing.
Wastewater surveillance can be used as an early indicator for the presence of infections not yet detected by traditional clinical surveillance, offering a picture of public health in the absence of symptoms and individual testing.
So how exactly is this wastewater surveillance carried out?
The Public Health Agency of Canada (PHAC) is working in collaboration with other federal departments, provincial, territorial and municipal governments and academia across Canada to establish a pan-Canadian wastewater surveillance network capable of monitoring the spread of COVID in Canada.
As COVID can be characterized by symptomatic and asymptomatic infection, it is important to identify the presence of undiagnosed cases to minimize the likelihood of outbreaks. Even a few days of early warning can be critical to the success of public health interventions and can be an imperative source of information for public health action.
Dr. Kimberley Gilbride is a professor and acting associated dean for the faculty of science at Toronto Metropolitan University (TMU) in Toronto, Ontario. Her lab is working to help to track the prevalence of COVID in local communities. Samples are tested from sites all over the city, including large treatment plants and community and congregate sites, such as university residences, shelters, and long-term care homes.
Does TMU’s procedure differ from other academic or public testing facilities?
According to Gilbride, most university labs are processing solids from raw wastewater, although a few are processing primary sludge, and a few are processing supernatant (the liquid lying above a solid residue after crystallization or precipitation). Her team has not seen a significant difference in detection between the sources or procedures as other labs doing similar work, as they have processed joint samples for comparison.
“In my lab, we process from raw wastewater and simply centrifuge the samples to collect the pellet (solids) and then extract for RNA [ribonucleic acid]. Although there are minor differences in the exact protocol between labs, the overall process is very similar,” explains Gilbride. “Different variants just require different primers for the RT-qPCR [reverse transcription quantitative real-time PCR] step. I think that every RT-qPCR reaction gives us accurate results, and all those using this analytical method get very similar results. However, the variation we see in detection — between samples, between labs, and between sites — is mostly due to the variation in the sample we are testing.”
What are they key challenges involved in providing accurate surveillance results?
The best way to explain this, according to Gilbride, is to imagine that wastewater is chicken vegetable soup. When you take a spoonful, you cannot guarantee that you pick up exactly the same number of carrots pieces each time. Even if you stirred the soup before portioning it into bowls, each bowl would not have exactly the same numbers of carrots or chicken in their bowl; hence, variation. The same thing happens with wastewater samples; some samples are more homogenous than others. (For example, poop comes in different consistencies and therefore single samples may vary.)
Gilbride adds that they normalize their COVID RNA copies with pepper mild mottle virus (PMMoV) since the latter is common in diets (but again may vary between different locations) and its presence in waste represents the amount of poop when analyzing for COVID.
“So, in other words, if we count chicken pieces in the soup, we can predict how much soup we are analyzing assuming the soup is homogeneous. Then, when we look for COVID, we determine how many carrots we have relative to chicken to see if the signal is going up, going down or steady. The challenge is always with the sample we get in the first place.”
How homogeneous is it? “It’s very hard to standardize unless we could get everyone to give us standardized poop samples — impossible! Having said all of this, the normalization with PMMoV has worked extremely well.”
Similarly, Metro Vancouver is working with the British Columbia Centre for Disease Control (BCCDC) and the University of British Columbia to track the presence of the COVID virus in the region’s wastewater.
Sableen Minhas, BCCDC’s communications specialist, says that their Public Health Lab (PHL) already had an existing collaboration, methods, and equipment for testing enteric viruses in wastewater prior to the pandemic, which meant the lab was able to quickly switch gears to test for COVID.
“The process to detect SARS-CoV-2 in wastewater usually involves collection of a sample from a wastewater treatment plant, preparation steps to concentrate and extract viral RNA and analysis for genetic markers of SARS-CoV-2 using quantitative, reverse transcription polymerase chain reaction (RT-qPCR),” says Minhas.
Wastewater is collected three times a week and the results are posted every Friday. Analyzing untreated wastewater samples is complex and takes longer than a typical lab sample. To get accurate results, multiple factors and samples need to be taken into account; the complete process includes collection, transportation, processing, testing, and analysis. An interactive map provides current data for those who want a snapshot of COVID virus trends for various areas in B.C.
Wastewater testing woes
As the science continues to evolve and studies continue to be critical of evolving scientific methods, some definitive pros and cons to wastewater testing have been revealed.
One comprehensive study conducted by Ontario’s Science Advisory Table, a group of scientific experts and health system leaders who evaluate and report on emerging evidence relevant to the COVID pandemic, has identified three challenges that warrant further consideration to ensure better wastewater testing reliability:
Analytic methods Approaches for sampling and measuring viral RNA vary considerably across jurisdictions, as do the populations surveyed and the sewer networks. There is a need for improved quality assurance between analytical methods, as well as consistency in data interpretation within local context.
Surveillance programs Most wastewater testing programs worldwide are still in the developmental stages, and while capacity is expanding, there is a need to transition to a sustainable system.
Collaboration elements Public health, testing laboratories, and wastewater utilities need to collaborate to ensure testing provides actionable public health intelligence which is interpreted and communicated and actioned effectively.
The study, which was published in August 2021, also notes that the PHAC, the WHO, the Centers for Disease Control and Prevention (CDC) and others have also identified analytic methods, reporting, and interpretation of tests and program sustainability as areas that require additional development.
The consensus is that wastewater testing as a surveillance tool for COVID is relatively new and requires ongoing development, standardization, capacity building, and sustainable infrastructure.
COVID wastewater surveillance working groups and dashboards
Cultivating quality assurance
There are organizations working to improve the development of quality assurance and early warning wastewater screening of COVID. The Canadian Water Network’s COVID-19 Wastewater Coalition, which brings together municipal utilities, researchers, public health agencies, and governments, is one such organization.
The COVID-19 Wastewater Coalition is sharing critical knowledge — and providing critical context — to accelerate progress and help ensure that surveillance results can be both sufficient scientifically rigorous and useful to public health authorities.
When Bernadette Conant, CEO of the Canadian Water Network, became aware of the emerging science around COVID she mobilized and led the launch of the coalition in March 2020. The coalition recognizes the need to marshal resources and help frame the discussion in Canada.
Together with a team of leading water experts, the coalition is focussed on answering a few key questions. First, does surveillance testing work? Yes, the caveat is always that there has to be a careful process. Secondly, can we trust the data? Mostly the answer is yes. The sticking point is that this is a new science, and has not yet passed to the accreditation stage. Finally, are the data useful or being used for public health decision making? That’s where it gets a little murky.
“Omicron really changed the conversation around, and greatly upped the interest in, wastewater surveillance,” points out Conant. “We were having a new wave and it quickly challenged the ability to keep up with PCR testing.”
Wastewater testing became more important for the ability of understanding how widespread omicron was in the community. Suddenly, says Conant, there was more confidence in the wastewater testing signals.
The coalition is a community of aligned experts who are helping to provide evidence informed decision making. Conant emphasizes the importance of providing context to the research and making accurate real-world decisions.
“One of the things that is in our new strategic plan and one of our strengths is being ‘context experts’ rather than ‘content experts.’ The coalition is helping to provide this service by getting the right people in the room at the right time and helping everyone feel involved,” explains Conant, who is passionate about providing clarity and guidance in this evolving environment.
Due to changes in COVID-19 testing policies in many jurisdictions starting in late December 2021, the PAHC warned that case counts would underestimate the total burden of disease.
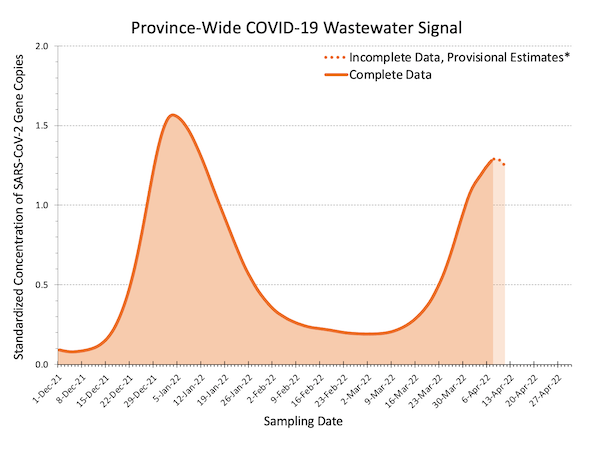
As we go to press, wastewater dashboards are suggesting a rise. The surge is mainly taking place in Quebec, Ontario, Alberta, Saskatchewan, and parts of British Columbia. There’s speculation over what that will mean — a sixth wave of the pandemic or a blip that is the beginning of the endemic? Public health is keeping an eye on infections, health impacts, and hospitalization rates.
Something is coming and we don’t know exactly what. In the meantime, let’s responsibly enjoy easing restrictions as wastewater surveillance continues to improve and provide a (relatively accurate) heads-up.
Connie Vitello is the editor of Environment Journal.